Dupuytren’s disease can be confusing because patients often receive different advice depending on which specialist they see. Knowing the right questions to ask can help you understand whether your condition is early or advanced, explore treatment options such as radiotherapy or surgery, and make informed decisions about managing progression and contracture.
When people are diagnosed with Dupuytren’s disease, they are often told very different things depending on which doctor they see.
That’s because different doctors deal with different stages of the condition, and if you ask the wrong questions, you can easily end up on the wrong pathway.
This guide breaks it down into three parts: what to ask your GP, what to ask a radiotherapy specialist if you are considering early treatment, and what to ask a hand surgeon if the disease is more advanced.
1. What to Ask Your GP
Is this actually Dupuytren’s disease?
Most of the time, Dupuytren’s is straightforward to diagnose. It has a very characteristic pattern, with a lump in the palm (a nodule), sometimes with a cord under the skin, and sometimes with dimpling or tightening of the skin.
In those typical cases, no further tests are needed.
If something doesn’t quite fit, it is reasonable to ask whether it could be something else, such as a ganglion or another type of lump, and whether an ultrasound would help clarify things.
Is this early or advanced Dupuytren’s disease?
This is one of the most important questions you can ask.
What you are really asking is whether there is a contracture, meaning that the finger is being pulled into a bent position, or whether this is still at an earlier stage where the fingers are straight or only slightly affected.
This distinction matters because early and advanced disease are treated in completely different ways.
What should I do about it?
This is where many patients are told to wait until the fingers bend and then consider surgery.
That is the standard NHS pathway, but it is not the only approach.
If you want to take a more proactive approach, it is reasonable to say that you do not want to wait for the condition to worsen, and that you would like to understand whether there are options to reduce progression, even if they are not available on the NHS.
Can you refer me to a doctor who treats early Dupuytren’s disease?
This is the key step.
If you are referred to a physiotherapist, MSK specialist, or hand surgeon, you will usually be placed on a pathway for advanced disease. If you want to explore early treatment options, you need to see a radiation specialist.
If your GP is unsure or hesitant, this is where you need to be clear and specific.
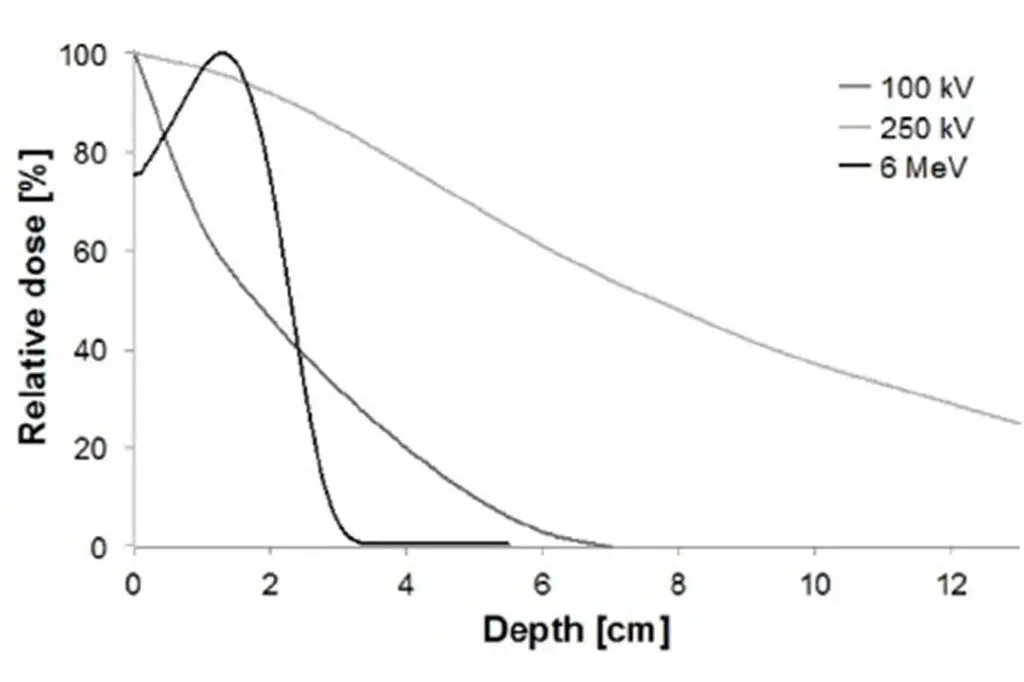
You can explain that radiotherapy is used at a much lower dose than in cancer treatment, typically around 30 Gray in total, compared to 60–70 Gray for cancer. The aim is not to destroy tissue, but to reduce the activity of the cells that drive Dupuytren’s disease.
You can also explain that the side effects are usually limited to the skin. Some people get redness, soreness, or dryness for a couple of weeks after treatment, and a proportion of people have some long-term dryness in the treated area, which is usually mild and manageable.
If the concern is about cancer risk, it is reasonable to explain that the risk is very low. For someone around the age of 50, the lifetime risk is around 1 in 1,000, and this is usually a type of skin cancer (called a basal cell carcinoma) that does not spread and is straightforward to treat. This needs to be balanced against the risk of the condition progressing and eventually requiring procedures.
You can also say that although radiotherapy is not funded by the NHS, it is permitted, considered safe, and supported by clinical evidence showing that it reduces progression.
Even if your condition is very early, it is still reasonable to ask for a referral. At the very least, you can get clear advice on how to monitor the condition properly and when to return for treatment if it becomes active.
2. What to Ask a Radiotherapy Specialist
What is your experience treating Dupuytren’s disease?
It is reasonable to ask how many patients they treat and how familiar they are with this condition, as experience makes a difference to both assessment and treatment decisions.
What dose and treatment schedule do you use, and why?
The standard approach is two phases of treatment, each delivering 15 Gray in five sessions, separated by a gap of around three months.
If a different schedule is suggested, you should ask why. There may be practical reasons, but you should understand the trade-offs.
Expert Non-Invasive Treatment for Dupuytren’s and Ledderhose Disease Across the UK
Dr Richard Shaffer set up Dupuytren’s UK in April 2011 to provide non-invasive treatments for people who suffer from benign conditions such as Ledderhose disease and early-stage Dupuytren’s contracture in the Guildford area. Today, Dupuytren’s UK offers this service to patients throughout the UK.
What area of the hand will you treat?
This is a critical question.
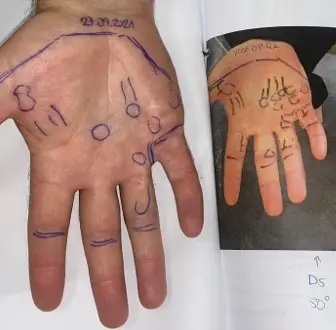
The treatment area should usually include the affected part of the palm and extend towards the fingers up to the middle joints, which are called the PIP joints. It should avoid areas that are not involved in the disease, particularly the fleshy parts at the base of the thumb and little finger, and it should avoid the wrist area.
If the treatment area is very small and only covers a single lump, there is a risk of missing areas that may become involved later. If it is very large and covers the whole hand, there may be unnecessary exposure.
You should expect a clear explanation of why the field has been chosen, and ideally this should be shown to you visually.
What should I expect during and after treatment?
Radiotherapy itself is straightforward and does not cause pain or make you feel unwell.
After treatment, the skin may become red, dry, or slightly sore, usually settling within a few weeks. You should be given clear advice on how to look after your skin and what activities to avoid while it is more sensitive.
You should also be advised on longer-term factors that may influence the condition, such as smoking, alcohol, and repeated strain or trauma to the hands.
What follow-up will I have?
You should understand how your condition will be monitored after treatment and what signs would suggest that further review is needed.
3. What to Ask a Hand Surgeon
Do I need treatment to release the contracture?
If the fingers are bent, the decision to treat depends on both the degree of contracture and how it affects your function.
Problems with everyday activities such as washing your face, putting your hand in your pocket, wearing gloves, or shaking hands are all important factors.
What type of procedure are you recommending?
Open surgery is the standard approach, but less invasive options such as needle aponeurotomy may be appropriate in some cases.
If this is not being offered, it is reasonable to ask whether it would be suitable for you and why it is not being considered.
What is the chance of recurrence, and can this be reduced?
Dupuytren’s disease can come back after treatment.
It is reasonable to ask how likely this is in your case and whether anything can be done to reduce the risk, including whether additional treatments such as radiotherapy might be appropriate.
What does recovery involve, and what are the risks?
You should understand whether the procedure is done under local or general anaesthetic, what recovery involves, and what the risks are.
These include nerve injury, tendon injury, infection, and bleeding.
What is your experience with this procedure?
It is always reasonable to ask how often your surgeon performs this procedure and what their outcomes are.
Final Thoughts: Asking the Right Questions Matters
Dupuytren’s disease is not a single pathway condition. Early disease, active disease, and established contracture all require different approaches and different types of expertise.
The most important thing you can do is make sure you are asking the right questions and seeing the right specialist at the right time. That is what allows you to make informed decisions and avoid being pushed down a pathway that may not be right for you.