Does private medical insurance cover radiotherapy for Dupuytren’s disease? Coverage varies between providers like Bupa, AXA, and Vitality. This guide explains what’s typically covered, how to get authorisation, and what to do if treatment isn’t included.
If you are considering radiotherapy for Dupuytren’s disease, one of the first questions is whether your private medical insurance will cover it.
Some patients are told by their insurer that the treatment is “experimental”, particularly where cover is not provided. This can create uncertainty, but in practice the situation is usually clearer once you understand how insurers approach this.
This guide explains which insurers are likely to cover treatment, what to do if your insurer raises concerns, and how to approach the process step by step.
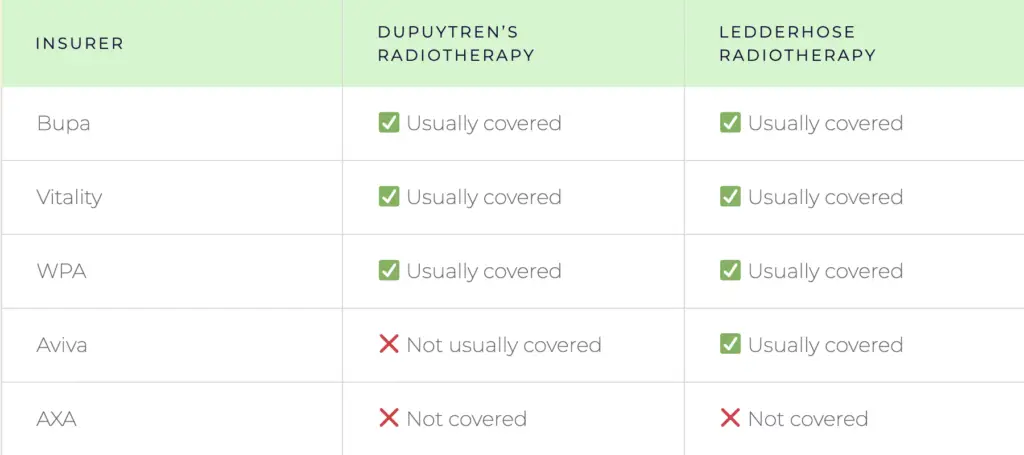
Which insurers cover radiotherapy for Dupuytren’s disease?
Coverage varies between insurers and largely determines your options.
If your insurer does not cover radiotherapy for Dupuytren’s disease, it is usually not a good use of time trying to pursue it through insurance. In that situation, it is more practical to ask about self-funding options so that you can decide how you want to proceed.
Action point
Check your insurer first – this will determine what pathway is available to you.
What to do if your insurer says the treatment is “experimental”
Occasionally, insurers will describe radiotherapy as “experimental”, particularly where they do not cover it. In practice, this usually reflects how the insurer has chosen to classify and fund the treatment, rather than whether it is used clinically.
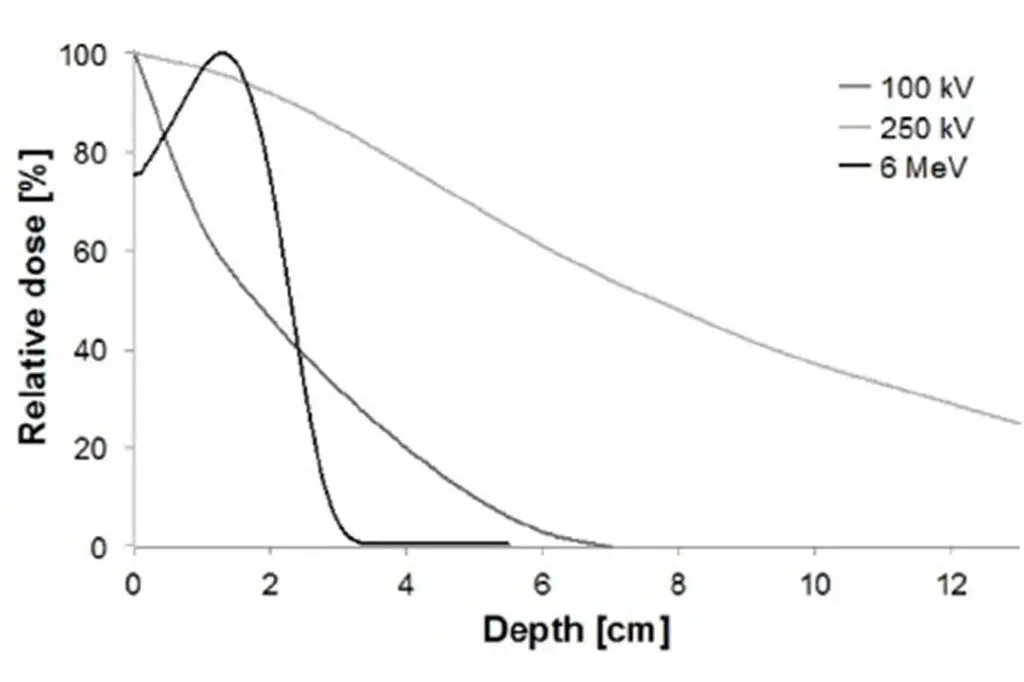
The more important question is whether radiotherapy is appropriate for your stage of disease. There are long-term studies showing that radiotherapy can reduce progression and reduce the likelihood of needing surgery when used in early, active Dupuytren’s disease.
Action point
Will my private medical insurance approve radiotherapy treatment?
Approval depends on stage and correct process
If your insurer covers radiotherapy, approval is usually straightforward when:
- the disease is early-stage and progressing
- radiotherapy is being used within standard clinical criteria
- the request is supported by a clinic letter and treatment plan
Common reasons for refusal
- the policy excludes Dupuytren’s disease or pre-existing conditions
- treatment is requested before a clinical assessment
- the disease is too advanced for radiotherapy to be appropriate
Action point
Expert Non-Invasive Treatment for Dupuytren’s and Ledderhose Disease Across the UK
Dr Richard Shaffer set up Dupuytren’s UK in April 2011 to provide non-invasive treatments for people who suffer from benign conditions such as Ledderhose disease and early-stage Dupuytren’s contracture in the Guildford area. Today, Dupuytren’s UK offers this service to patients throughout the UK.
You only need authorisation for the initial consultation first
A common source of confusion is trying to get treatment authorised before you have been seen.
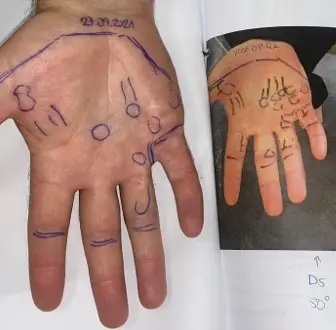
At the beginning, all you need is authorisation for an initial consultation. That allows a proper assessment to take place, including confirming the diagnosis, understanding how active the disease is, and deciding whether radiotherapy is appropriate.
Action point
The clinic will provide what is needed for authorisation
If radiotherapy is recommended after your consultation, the clinic will provide the necessary information to support authorisation. This includes a clinic letter outlining the diagnosis and treatment plan, along with the appropriate radiotherapy codes.
If the insurer requires additional information, this can also be provided.
Action point
If your insurer doesn’t cover treatment
Action point
If treatment is not covered, consider whether you want to self-fund. You can see a guide to self-funding costs here.
Summary: How to approach insurance for Dupuytren’s radiotherapy
Follow these steps
- Check whether your insurer is likely to cover treatment
- Get authorisation for an initial consultation
- Attend the consultation to assess suitability for radiotherapy
- Apply for treatment authorisation
- If not covered, consider whether to self-fund