If you’ve found a lump in your hand and have a family history of Dupuytren’s disease, it’s natural to worry. While the condition often runs in families, it doesn’t always progress the same way. This guide explains early signs, risk factors, and when to monitor or consider treatment.
If your parent has had Dupuytren’s disease and you’ve now found a lump in your own hand, you may wonder what this means for you. Many people worry that the condition will develop in the same way, especially if they have seen a parent get contractures of their fingers or have invasive surgery. But while Dupuytren’s often runs in families, it doesn’t follow a fixed pattern, and it can vary a lot from one person to another.
It may be that no-one in your family has had Dupuytren’s disease as Dupuytren’s can skip generations, or be so mild that it was never diagnosed. Despite this, around 80% of the risk of developing Dupuytren’s is genetic, and of course you cannot change your genes! But what you can do is understand the condition properly and be aware of the factors that can influence how it behaves.
How Family History Affects Your Risk
Dupuytren’s is best thought of as something you can be prone to, rather than something that is guaranteed to develop in a particular way. Doctors sometimes use the term “diathesis” to describe this underlying tendency. In Dupuytren’s, this refers to a group of features linked to a higher chance that the condition may be more active and get worse over time. These include a clear family history involving a parent or sibling, disease in both hands, the presence of knuckle pads, involvement of the feet (Ledderhose disease), onset before the age of 50, and being male.
The more of these features that are present, the higher the risk of the condition getting worse with time. But it still doesn’t allow us to predict exactly what will happen in a particular person. You might have only one of these features and still find that it gets worse, or you might have several features and find that things remain stable for many years. Finding a nodule at a younger age can be relevant, but on its own it does not tell us how the condition will behave. A more useful way to think about Dupuytren’s is that it can be a long-term tendency that needs watching as it evolves, rather than something that will definitely get worse.
What an Early Lump in the Hand Means
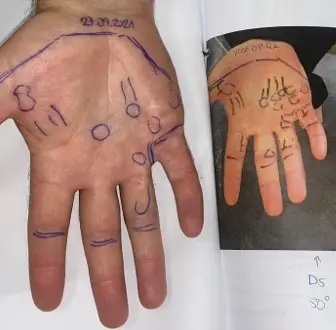
The key signs of Dupuytren’s are nodules, cords, and skin retraction. In the early stage, people usually have nodules, sometimes with early cords and mild skin changes, but without a clear contracture (fixed bending of the finger) affecting function. Many people reading this article will be at the earlier end of that spectrum, where there is a lump under the skin and maybe thin cords towards the wrist or fingers, but no obvious fixed bending (contracture) of the fingers.
At this stage, the main issue is not the fact that you have a lump, but whether it changes. It may grow, extend, or become associated with a cord. The presence of a nodule on its own doesn’t tell you what will happen next, but it is definitely something to keep an eye on rather than ignore.
Expert Non-Invasive Treatment for Dupuytren’s and Ledderhose Disease Across the UK
Dr Richard Shaffer set up Dupuytren’s UK in April 2011 to provide non-invasive treatments for people who suffer from benign conditions such as Ledderhose disease and early-stage Dupuytren’s contracture in the Guildford area. Today, Dupuytren’s UK offers this service to patients throughout the UK.
What Changes to Look for Over Time
The most important question is whether things have changed, particularly over the last 6–12 months. Signs that things are becoming more active include new nodules appearing, existing nodules getting larger, cords forming or extending, or your hand starting to feel tight. You may also notice that it’s more difficult to bend your fingers back, or even that you can’t fully straighten your fingers.
Some of these changes are subtle and may not be completely obvious as they can develop slowly. For this reason it’s worth having your hands assessed properly. This gives you a clear starting point, so that if you think something has changed later, it can be checked objectively rather than just relying on memory.
How Age and Family History Affect Progression
Age and family history are most useful when you consider them together. If you are younger, male, and have a family history of Dupuytren’s, the condition is more likely to become active at some point, and this links to the idea of diathesis that I described above. Even so, there is still a wide range of possible outcomes. Some people find that things change quite quickly, which may be followed by long periods where nothing happens, while others find that progression is more steady as the condition develops.
So there is no single path that everyone follows. Being aware of the condition and watching how it behaves is much more useful than trying to predict exactly what will happen in your particular case.
Looking After Your Hands
If you do have early Dupuytren’s, you should be aware of factors that may make it more likely to get worse. A lot of heavy gripping, high-force activities, impact, and vibration can make things worse, particularly if these are frequent or intense. This doesn’t mean that you need to stop doing what you enjoy, but it is worth thinking about how to protect your hands better where possible.
Also, Dupuytren’s is more likely to get worse if you smoke, and drinking alcohol can also increase risk, even at moderate levels, although smaller amounts are likely to have less of an effect. If you have diabetes, keeping it well controlled is important. As an added bonus, improving all these things is important for your general health as well as for Dupuytren’s.
When to Monitor and When to Consider Treatment
Not all early Dupuytren’s disease needs treatment. In many people, especially when there’s no clear change and no impact on function, the right approach is just to keep an eye on it. You should consider being seen early by a doctor who specialises in early Dupuytren’s disease, as this will help you understand what you are dealing with and give you a clear baseline for comparison.
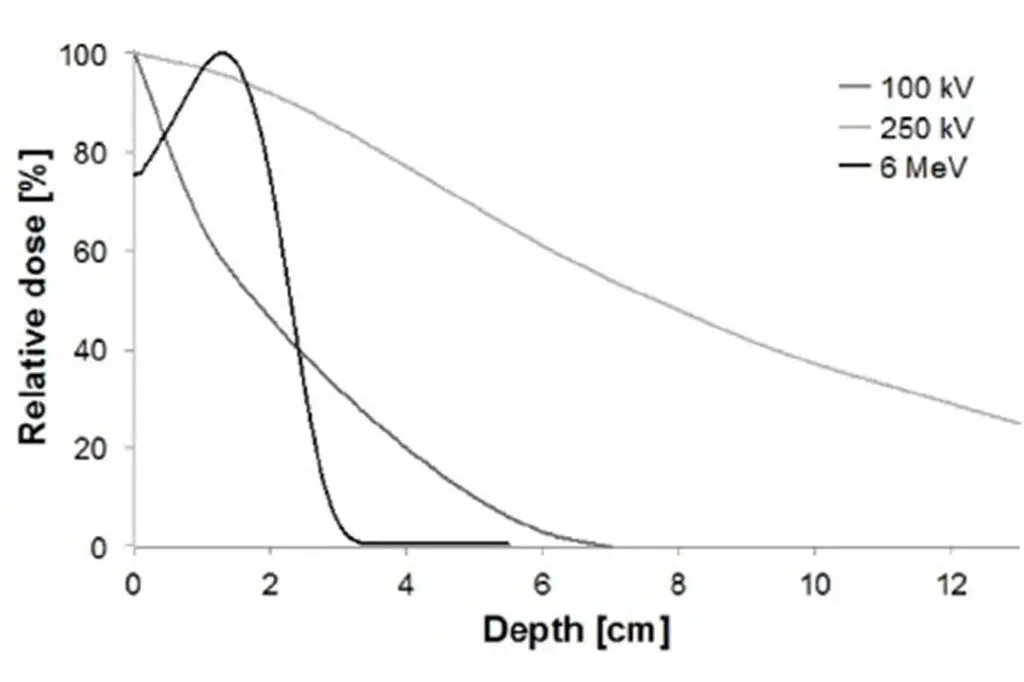
If you notice that things get worse (like increasing nodules, cords, skin changes, or early effects on movement), then you may want to consider active treatment with low-dose radiotherapy. This treatment is used where the condition is becoming active, and the aim is to stabilise the situation and reduce the chance of it getting worse still, and ultimately prevent the need for invasive surgery. The key is choosing the right window of opportunity, so that treatment isn’t given too early and isn’t given too late.
What to Do If You’ve Found a Lump
Not all early Dupuytren’s disease needs treatment. In many people, especially when there’s no clear change and no impact on function, the right approach is just to keep an eye on it. You should consider being seen early by a doctor who specialises in early Dupuytren’s disease, as this will help you understand what you are dealing with and give you a clear baseline for comparison.
If you notice that things get worse (like increasing nodules, cords, skin changes, or early effects on movement), then you may want to consider active treatment with low-dose radiotherapy. This treatment is used where the condition is becoming active, and the aim is to stabilise the situation and reduce the chance of it getting worse still, and ultimately prevent the need for invasive surgery. The key is choosing the right window of opportunity, so that treatment isn’t given too early and isn’t given too late.